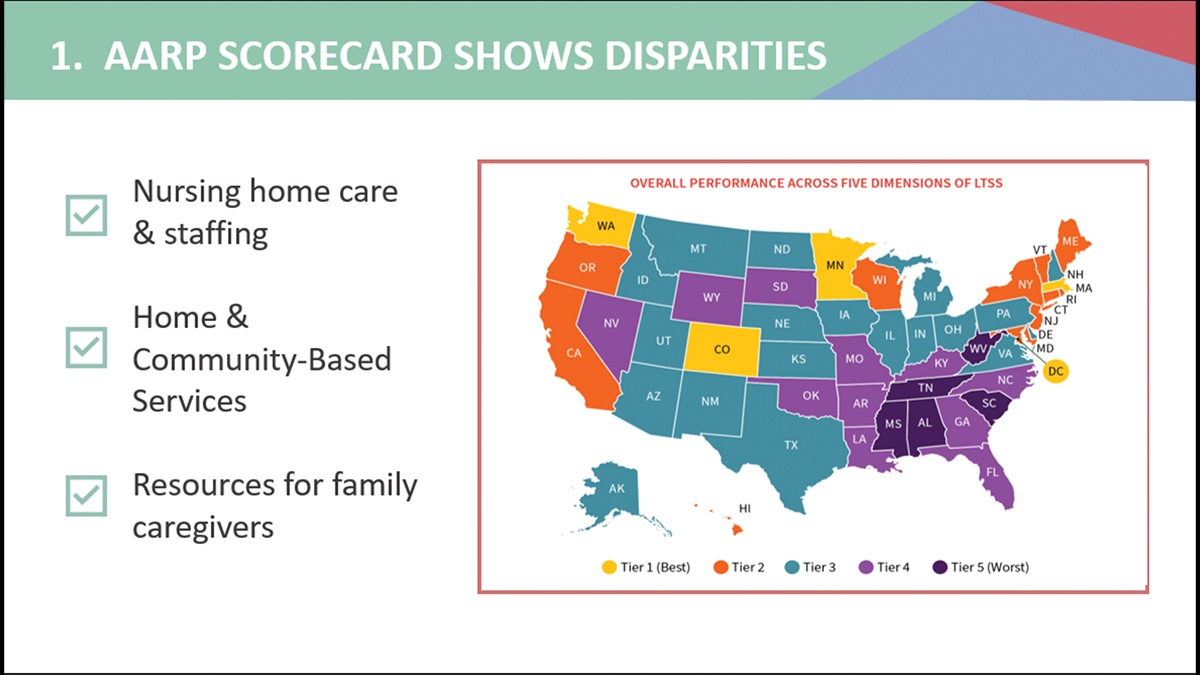
Caregiving is a job that doesn’t discriminate. However, millions of America’s long-term caregivers battle low or no pay, discrimination based on race and gender, and an overall lack of respect for the vital service they provide.
Journalists covering long-term caregiving must carefully analyze the demographics of this critically important workforce. According to AARP’s Executive Vice President and Chief Advocacy & Engagement Officer Nancy LeaMond, 60% are women, 40% are people of color, 30% are millennials or Gen Z, and close to 30% of family caregivers are caring for both a parent and a child. Also, 10% are over the age of 80.
LeaMond, along with National Domestic Workers Alliance President Ai-jen Poo, urged National Press Foundation fellows to thoroughly explore the nuances of the long-term care workforce. The following quotes are highlights of their session:
Ai-jen Poo:
“I was raised in an intergenerational household, an immigrant family, where my grandparents played a huge role in raising me. And both my mom and my grandmother were in caregiving professions on top of caring for my family, and all the aunties and uncles and all the people who I thought were my blood relatives, but actually were just members of the community.”
“As they all grew older, my grandparents in particular, as they aged and needed more support—the struggles that my family faced to find appropriate caregiving for them really showed me the range of scenarios in the Wild West of this caregiving reality. From my grandfather ending up in a nursing home room, where he shared a room with six other people, had food that was unrecognizable, the lights didn’t even work in the facility, and the workers were responsible for about 20 people each.”
“To my grandmother, who was able to live independently in her home for about a decade, going to church twice a week, playing Mahjong, really living life on her terms, until she had a stroke. Because she had the support of both family caregivers and home care workers, that there’s just a whole range of both what’s possible and what we’re missing. That became my obsession and especially the people who are really passionate about caring for others, like my grandmother and my mom and the millions of family caregivers and direct care workers out there, how do we get them the support they need to care for themselves and the rest of us.”
“And so, 25 years ago, we started organizing first in New York in church basements. And today, we are a community of about 400,000 home care workers, nannies, and cleaners around the country, in every state. And we’ve passed some legislation to protect the rights of this workforce in 10 states and four cities. And in 2011, we launched a campaign with Jobs With Justice called Caring Across Generations, which is meant to bring together family caregivers, workers, and people who need care and support to develop big, bold solutions to help more people get access to the care they need and more workers have good jobs, who provide that care.”
So yes, we’re going to have more people living with chronic illnesses, and yes, it is also possible to live well, but some change is going to be required to support that. And I think that’s what we really need some storytelling on, is what are the policies, what are the shifts in our culture and the way that we think about aging and living well, the way we think about care teams. That caring, it’s not just either family members or a workforce, it’s both and—how do we support all of those caregiving relationships that are going to help enable us to live well as we live longer.
Nancy LeaMond:
“There are roughly 55 million people in this country now over the age of 65. And then, we use 2040, there’ll be 80 million. So, think about that growth in the number of people over the age of 65. But also, we have a vision of people over the age of 65, and many of us are a little healthier, more vibrant than you might remember your grandparents growing up.”
“The truth is one-third of people over the age of 65… have some kind of cognitive impairment or some kind of dementia. 95% have at least one chronic condition. And so, there are more people over the age of 65. There are more people living with chronic conditions that require, frankly, a lot of care. And the number of people getting illnesses such as dementia, Alzheimer’s, Parkinson’s, ALS, MS is growing dramatically.”
“I’ve been a serial caregiver. I was somebody who helped my mother take care of my father. When my father passed away, I’m an only child, I took care of my mother remotely. She lived in New Jersey. And then, about, I guess eight, nine years ago, my husband was diagnosed with ALS. And we made the decision to have him stay in our home, and we did six years of caring. He was incapacitated from almost the day of diagnosis, so required some care. And it really was as Ai-jen described. I was a caregiver. My two millennial sons were caregivers. And we had five or six paid caregivers as a part of it.”
“I remember when my husband was first diagnosed, I went to some of the AARP materials, and most of the materials were how to make sure your loved one doesn’t wander away, doesn’t go out the front door. My issue was not my husband wandering away. My issue was how can I lift him up, how could I help him get out of a chair. And so, my experience was in that area. Others are in others. As an organization, we work very hard to provide a set of information and tools for people as they become caregivers.”
“Make no mistake, money helps. And in Washington, D.C. full-time, 24/7, home care is $180,000 a year. If you can’t do that, then you have to find a way to patch together, whether it’s through family, caregivers, friends, whatever, a way to take care of your loved one.”
Access the full transcript here.
The America’s Long-Term Care Crisis Fellowship is sponsored by AARP, which also sponsors the AARP Award for Excellence in Journalism on Aging, accepting applications until Oct. 16. NPF is solely responsible for the content.