The breakthroughs on cancer therapies have been fast over the past decade, with new forms of immunotherapy giving hope to patients who previously had been failed by any other treatments.
The question now becomes: Will vulnerable populations, who are not always now getting proper care, have access to those?
Brian Rivers, director of the Cancer Health Equity Institute at the Morehouse School of Medicine, told National Press Foundation fellows that while the racial gaps in diagnosis and treatment of some cancers are narrowing, they remain in others. And in some, the disparities in outcomes are alarming. As one example: African American men with prostate cancer are almost twice as likely to die as white men with the disease.
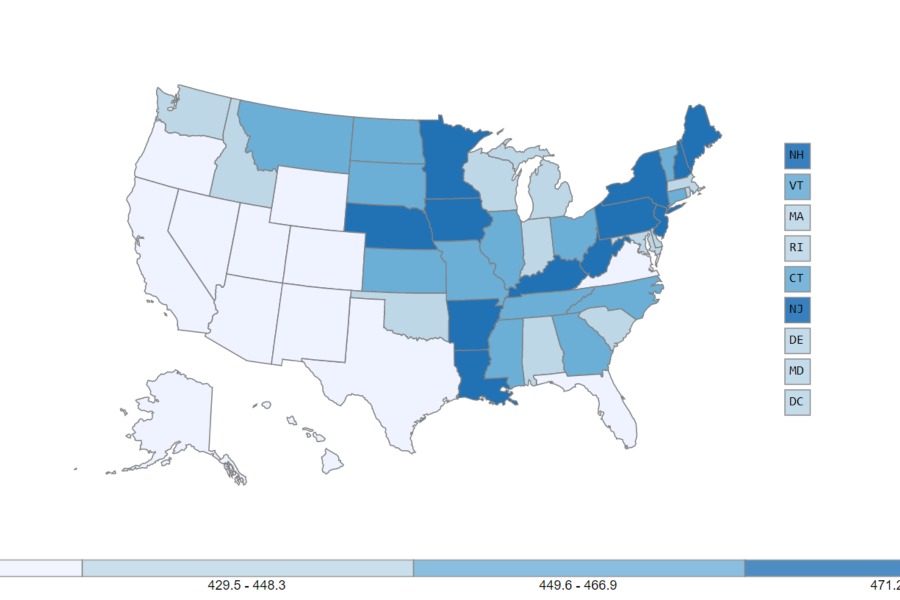
Among men, cancer incidence rates by race and ethnicity are highest in African Americans (540 per 100,000 men) followed by whites (501), Native Americans (399), Hispanics (372) and Asian/Pacific Islanders (292). Among women, the spread is not as wide and is topped by whites (441), followed by African Americans (407), Native Americans (371), Hispanics (333) and Asian/Pacific Islanders (290).
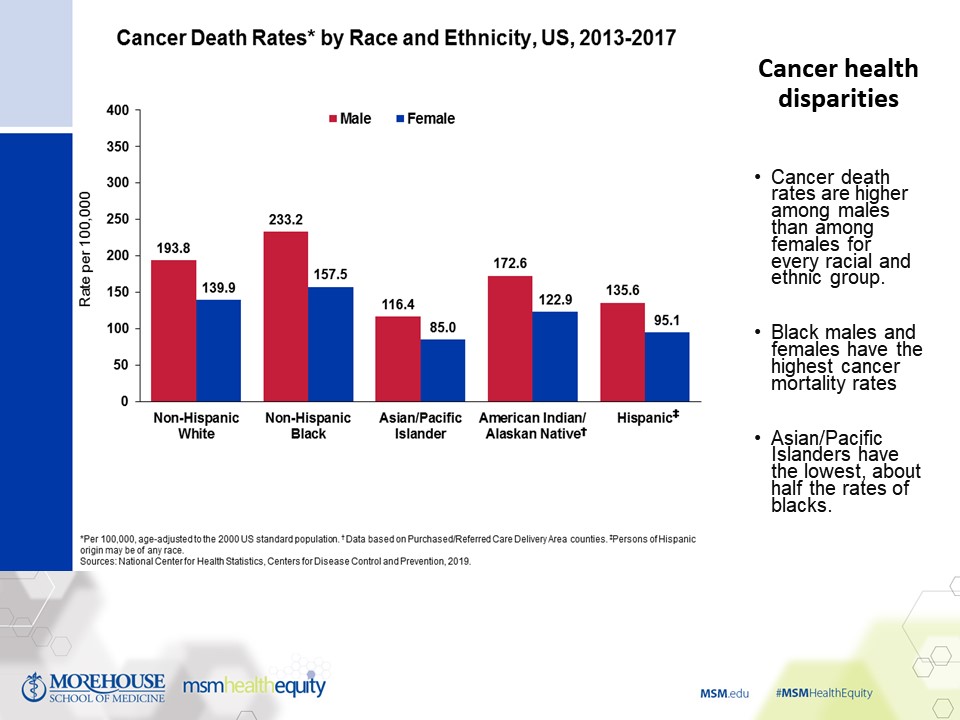
For deaths, African Americans top both gendered lists, and the gaps are wider – reflecting a lack of access to care, as well as to the quality of care received. An example: African Americans with multiple myeloma are 21% less likely than whites to receive the molecularly targeted therapeutic bortezomib – an important treatment.
An equally vexing problem, Rivers said, is the lack of African Americans and other non-white subjects in clinical trials.
“Today’s medicine is yesterday’s research,” Rivers said. “Our medicine and our medical enterprise is only as good as those who participated in helping generate the data that helps drive medicine. To have the participation of minorities will ensure that we’re able to best deliver quality care to the individual.”
The reasons for lack of minority participation in clinical trials are many and go back decades. Mistrust is still an issue – both of researchers and the health care system generally. Some of the reasons are practical: lack of transportation for some populations, and a lack of education about the clinical trial system.
Rivers cited one study that asked respondents if they trusted their doctors to “fully explain” a research study to them; 42% of African Americans said no or that they didn’t know, while only 23% of whites felt the same way.
This program is funded by the American Association for Cancer Research. NPF is solely responsible for the content.