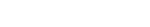Cancer is a complicated, multifaceted disease, and researchers are still working to understand how it develops.
But they know plenty of ways to prevent it: stop smoking, lose weight, exercise more, and drink less alcohol – and live in states that offer better medical care for all residents.
That was the assessment from Dr. Otis Brawley, a professor of oncology and epidemiology at Johns Hopkins University and the former chief medical and scientific officer of the American Cancer Society. He’s also the author of “How We Do Harm: A Doctor Breaks Ranks About Being Sick in America.”
“We could reduce cancer deaths 60% by paying attention to known risk factors,” Brawley told a group of National Press Foundation fellows.
Smoking is responsible for lung cancer, of course, but it’s also been linked to 16 other cancers, including stomach, bladder and kidney. Smoking rates have come down dramatically, but about 14% of Americans still smoke.
“If we just started getting to everybody, it has the prospect of saving more lives than any blockbuster drug,” he said.
The other way to control cancer is by making the health system more uniform, Brawley said.
There are vast difference in cancer outcomes by geography, as well as by race and income. However, the differences in outcome by race are driven by sociological factors – including income and education – and not biological differences between the races. The factors that matter stem from the area of geographical origin of one’s ancestors, not one’s race.
“We find populations that tend to do better than others,” he said. “Some populations are getting inadequate care – prevention, screening diagnosis, treatment.”
Overall, the U.S. has seen a 40% decline in age-adjusted female mortality from breast cancer from 1990 to 2016. But some states, such as Massachusetts, have seen breast cancer mortality drop twice as fast as others, such as Georgia, Brawley said.
This presents “vast opportunities to reduce the cancer burden” – even without new technologies or treatment – by getting the best, evidence‐based care to all Americans.
“If all Americans had the risk of cancer death as that of college-educated Americans, 132,000 of them would not have died,” he said.
“If you’re a 60-year-old man, your risk of dying from colorectal cancer is half what it was in 1980,” he said. “But why has there been a decline of 63% in Massachusetts but only 12% in Mississippi? That’s my concept of a serious disparity.”
This program is funded by the American Association for Cancer Research. NPF is solely responsible for the content.